Microwave ablation close to Vena Cava Inferior and Left Portal Vein
Microwave ablation of an unfavorably located lesion in segment I of the liver with a distance of only 4 mm to the vena cava inferior and a distance of 3 mm to the left portal vein. Follow-up Gadoxetate enhanced MRI showed expected postinterventional change with diminished intracellular uptake of the contrast agent without any trace of residual tumor.
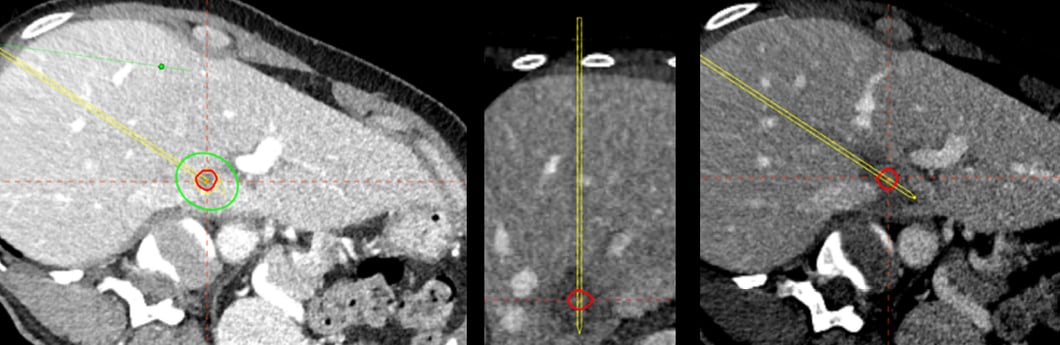
Postoperative control shows an almost perfect match between planned and treated tissue (middle and right).
Name: PD Dr. Anja Lachenmayer & Prof. Dr. Dr. Martin Maurer
Institution: Inselspital Bern
Patient age and sex: 52 years, female
Initial condition:
- Invasive ductal carcinoma (estrogen receptor 60%, progesterone receptor 5%-20%, Ki67 25%, HER positive)
- Subsequent FDG PET-CT showed an active lesion in the caudate lobe of the liver
- The final tumor stage was T2, N0, M1
Treatment:
-
Due to the unfavorable location in the caudate lobe ( Fig. 1 ) with a distance of only 4 mm to the inferior cava vein and a distance of 3 mm to the left portal vein surgery would be invasive and extensive. As the lesion was located just between the left portal vein and the vena cava inferior, it would have been very difficult even for an experienced interventionalist to position the ablation probe precisely within the lesion while not risking to in jure the vessels and otherwise to ensure a full therapeutic coverage of the lesion. Therefore the navigation system CAS-One was used to perform the procedure.
- Microwave ablation was applied as planned with a power of 100W for 2 minutes. Immediate postinterventional contrast enhanced control scan ( Fig. 2 B) revealed an ablation area of 30 ×16 mm, exactly as planned and fully covering the initial lesion also providing an adequate safety margin. The inferior vena cava and the left portal vein were not affected.
Conclusion:
- The 3- and 6-month follow-up Gadoxetate enhanced MRI showed expected postinterventional change with diminished intracellular uptake of the contrast agent (Fig. 3 B) without any trace of residual tumor also considering MR sequences of contrast dynamic and diffusion-weighted imaging.
Publication: Radiology Case Reports, Volume 14, Issue 2, Februar 2019, Pages 146 - 150


